Darelle Moffett is a midwife in the Rotunda Hospital in Dublin, where almost 10,000 babies are born each year.
Helping out on her family’s dairy and beef farm in Co Cavan, she was very familiar with birth and new life as she grew up.
“Calving was always a topic discussed at the dinner table,” she says. “A lot of people wouldn’t be used to that but it’s second nature when you live on a farm.”
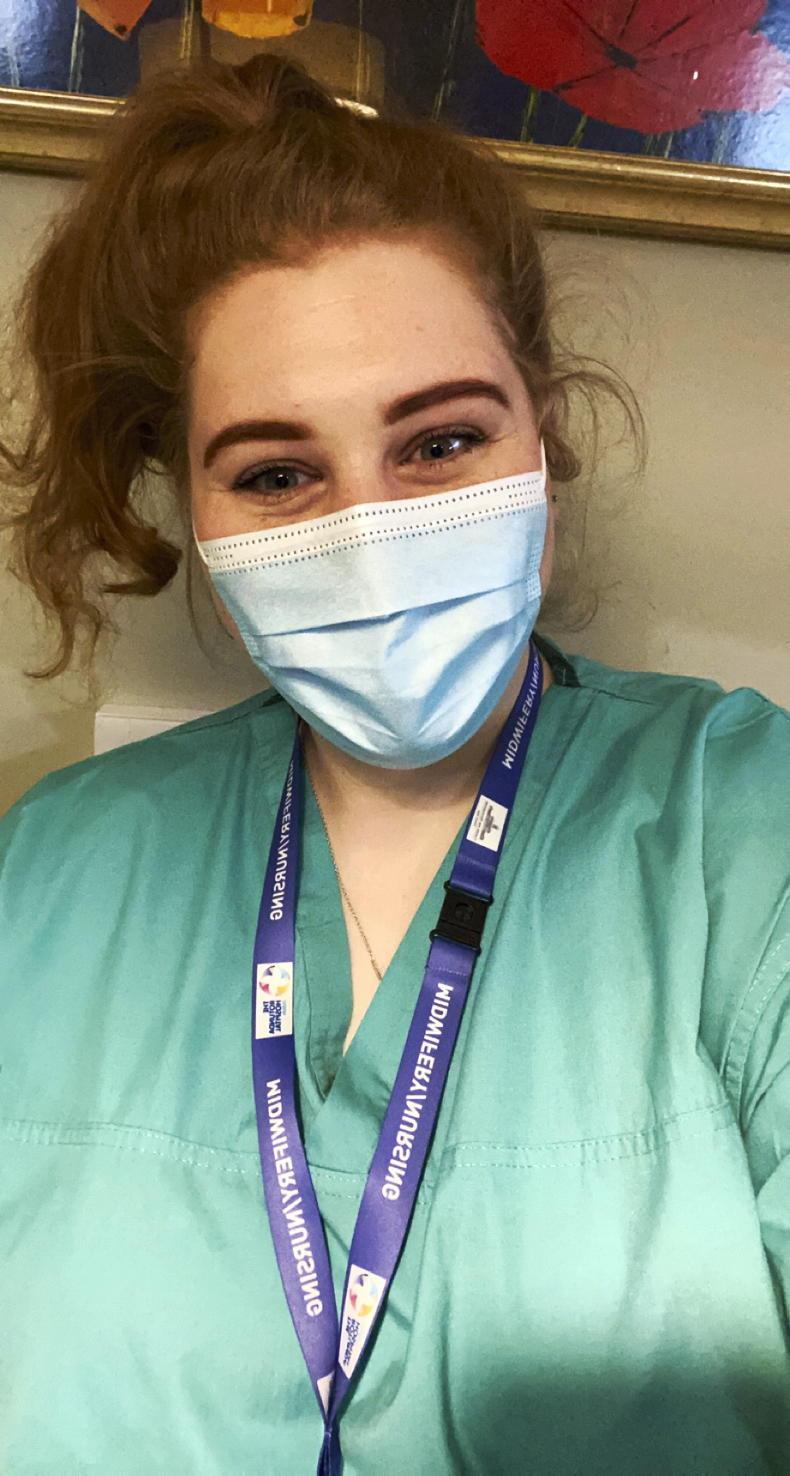
Darelle Moffett is a midwife at the Rotunda Hospital in Dublin.
It was while she was doing a work placement in a maternity hospital during her four-year nursing degree that she realised she wanted to be a midwife.
“The minute I walked in I thought, ‘This is for me’,” she says. “I worked with some amazing midwives who explained to me that these pregnant women are not sick; they’re just having babies. This was a mind-blowing concept to me, coming from a general hospital background where people are sick or have been in accidents. This completely flipped all that on its head to a really positive, exciting time.”
Autonomy of midwifery
Darelle was also attracted to the autonomy that midwives have.
“A woman can go through her entire pregnancy – until six weeks after the birth – only seeing her midwife (and not other medical professionals) if she is healthy and her pregnancy is low risk,” she says.
One midwife I met in training had cared for one woman in all her five pregnancies
“The autonomy of that really drew me to the role. A doctor or obstetrician only steps in if there is something wrong. It’s like in farming – you only call the vet when there is an emergency.”
Darelle liked the multicultural aspect of her work as well, looking after pregnant women from many countries and cultures, and the continuity of care in the job appealed to her.
“One midwife I met in training had cared for one woman in all her five pregnancies. I found that incredible. It’s a bit of continuity that I never knew before.”
Interview stress and success
Darelle did her interview to get a place on the post-grad midwifery course 18 months after qualifying and remembers the day of the interview very well – thanks to cows.
“I was milking that day, as my parents were away, so I milked really early in order to get to Dublin on time,” she recalls. “But didn’t half our cows break into our neighbour’s field and I had to get them rounded up and back into the field before hopping in the car, so I was a bit flustered by the time I got there!”
Explaining the morning she had to the interview panel didn’t do her any harm however, as she was accepted for the course, which began five months later.
Unforgettable day
Darelle’s biggest memory of midwifery, so far, has been the day she delivered twins.
“I’ll never forget that day as long as I live,” she smiles. “The mother was fully dilated at 10cm when she came in, so it was panic stations, but we had everything set up and her first baby was born very soon; a lovely baby girl.
I delivered the little boy. The absolute delight in the room was infectious
“There were a couple of midwives and obstetricians in the room and the senior midwife then told the doctors to step back and let the midwife deliver the second baby, too.
“That was me and I delivered the little boy. The absolute delight in the room was infectious. You can’t describe the happiness and relief after the weeks of waiting for these babies. To leave the room that morning, seeing the mother smiling with her two babies in her arms was incredible. It’s making me a bit emotional just thinking about it!”
There is extra joy, too, for midwives and families, when safe deliveries are long-awaited.
“You get women who have had a couple of losses and this is their rainbow baby that comes into the world and everything is healthy and, well, that’s amazing to see, as well.”
Lows and highs
There are difficult days too, of course.
“With incredible highs of course there are lows,” she adds. “There can be pregnancy loss and late-term pregnancy loss, which unfortunately is part and parcel of life. Then, of course, you have other issues in all hospitals, like short staffing, and there are always emergencies and a little bit of panic at some point throughout the day.
The positives far outweigh the negatives
“But it all comes as part of working in a clinical setting. The team I work with in the Rotunda is amazing, though. That makes all the difference, so I’m very lucky.”
Darelle has no trouble summing up her attitude to her job: “The positives far outweigh the negatives. You come home after the busiest day but you know that somewhere you’ve made a difference to someone’s life.”
And yes, Darelle loves babies. “You wouldn’t do this job if you didn’t!” she says.
Irish Farmers Journal as a remedy
A colleague (who commuted from Cavan) would bring Darelle a copy of the Irish Farmers Journal during the lockdowns, which helped her cope with homesickness.
“She knew that it was hard to get the IFJ around Stoneybatter,” she says. “I really appreciated being able to sit of an evening, cup of tea in hand, reading it, feeling that bit of nostalgia and homeliness.”
Emily McAteer lives on a suckler farm near Nobber in Co Meath with her husband and parents and, at the time of this interview, it was a case of “the labour ward at work and the labour ward at home” as calving was still happening.
As with Darelle, growing up on a farm normalised birth for Emily, who is now a clinical midwife manager in Our Lady of Lourdes Hospital in Drogheda.
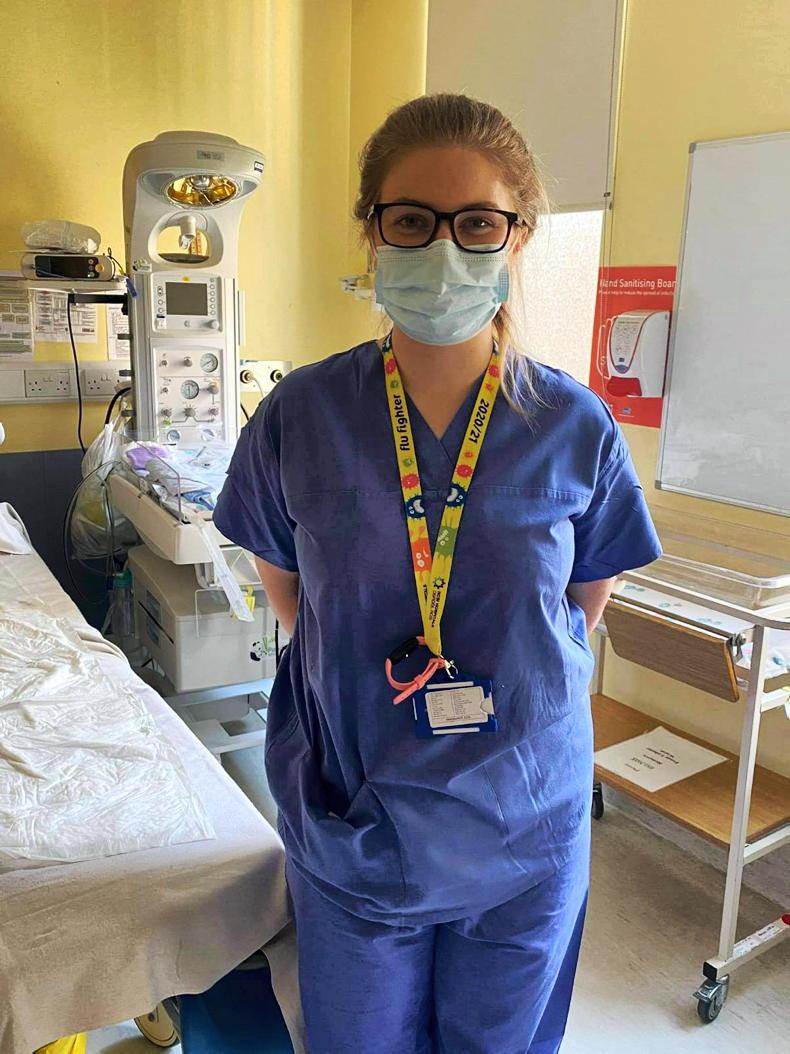
Emily McAteer is a midwife who lives on a suckler farm near Nobber, Co Meath.
“You’d be used to seeing cows calving and mares foaling, so birth was very familiar,” she says.
Emily went straight into midwifery training when she was 17 years old.
“I’m a direct-entry midwife and started my four-year course in midwifery in Dundalk IT,” she explains. “It’s a FETAC Level 8 degree. It’s an option that has been in existence for 10 years now, and mature students can apply, too. With this, you’re specialising straight away so it’s great if you’re sure that it’s what you want to do.”
Emily had a positive role model for midwifery in her family – her aunt had trained as a midwife in the UK. She also liked the insight into midwifery that the then-new TV series Call The Midwife provided, although she admits she may have had a slightly romanticised idea of the career.
I never thought of the complications that can arise – how unwell women can become at times
“At 17, you don’t have much life experience really,” she says. “Call The Midwife portrayed this kind of lovely normal and I only thought of normal birth, I suppose. I never thought of the complications that can arise – how unwell women can become at times.
“On-the-ward experience opened my eyes about how important our role is. Midwives are experts in normal pregnancy and labour, but you’re so important because you are the one that’s first detecting a deviation from that norm. You’re escalating it then and liaising with your multi-disciplinary team.
I just fell in love with midwifery
“That’s when your obstetric doctors come into play. I didn’t grasp all of that, initially, but getting a labour ward placement very quickly was a blessing. I felt like I got into the thick of it straight away. I just fell in love with midwifery then. It was an amazing experience and I think you know very quickly if it’s for you or not.”
Team effort
Emily qualified at the age of 21. “It is a lot of responsibility quite young,” she says, “but you have great support and, by that stage, you know what you’re about. It’s also very much a team effort here, with doctors and midwives working closely together. The autonomy you have is nice too.”
She also mentions the multicultural aspect of her job. “Ireland is such a diverse country now. We look after women from all over the world, so you learn about different cultures in relation to childbirth as you go.”
Emily believes that midwifery is a respected role and she is glad to see that men are now taking up midwifery as a career too.
“Midwife means ‘with woman’. You don’t have to be female to support a woman in childbirth. We need both sexes.”
Would do it all again
Emily has no doubt but that she would do it all again.
You just want to do your best
“The job is so rewarding. There are highs and lows like in any job but even on sad days you’re privileged to be in that room, supporting couples through. You are very much in the moment and you think, ‘If I was in this scenario how would I want to be treated?’
“That’s how I work,” she says. “You just want to do your best on the day for them. There are some very tough days, but women are amazing; so resilient and so strong. It’s a fantastic job.”
Pandemic challenge
The pandemic hasn’t been easy for midwives or new parents.
They both found the wearing of masks and PPE a huge challenge during the pandemic – for themselves and for new mothers.
“I suppose we’re all still a bit in shock about how it all occurred,” Emily says, “and it’s still ongoing but women and their families helped us so much by just being patient. It was so hard for new mammies and daddies with visitor restrictions as well but we look forward to it easing over time.”
Wednesday 5 May was the International Day of the Midwife.
For information about becoming a midwife click here.
Darelle Moffett is a midwife in the Rotunda Hospital in Dublin, where almost 10,000 babies are born each year.
Helping out on her family’s dairy and beef farm in Co Cavan, she was very familiar with birth and new life as she grew up.
“Calving was always a topic discussed at the dinner table,” she says. “A lot of people wouldn’t be used to that but it’s second nature when you live on a farm.”

Darelle Moffett is a midwife at the Rotunda Hospital in Dublin.
It was while she was doing a work placement in a maternity hospital during her four-year nursing degree that she realised she wanted to be a midwife.
“The minute I walked in I thought, ‘This is for me’,” she says. “I worked with some amazing midwives who explained to me that these pregnant women are not sick; they’re just having babies. This was a mind-blowing concept to me, coming from a general hospital background where people are sick or have been in accidents. This completely flipped all that on its head to a really positive, exciting time.”
Autonomy of midwifery
Darelle was also attracted to the autonomy that midwives have.
“A woman can go through her entire pregnancy – until six weeks after the birth – only seeing her midwife (and not other medical professionals) if she is healthy and her pregnancy is low risk,” she says.
One midwife I met in training had cared for one woman in all her five pregnancies
“The autonomy of that really drew me to the role. A doctor or obstetrician only steps in if there is something wrong. It’s like in farming – you only call the vet when there is an emergency.”
Darelle liked the multicultural aspect of her work as well, looking after pregnant women from many countries and cultures, and the continuity of care in the job appealed to her.
“One midwife I met in training had cared for one woman in all her five pregnancies. I found that incredible. It’s a bit of continuity that I never knew before.”
Interview stress and success
Darelle did her interview to get a place on the post-grad midwifery course 18 months after qualifying and remembers the day of the interview very well – thanks to cows.
“I was milking that day, as my parents were away, so I milked really early in order to get to Dublin on time,” she recalls. “But didn’t half our cows break into our neighbour’s field and I had to get them rounded up and back into the field before hopping in the car, so I was a bit flustered by the time I got there!”
Explaining the morning she had to the interview panel didn’t do her any harm however, as she was accepted for the course, which began five months later.
Unforgettable day
Darelle’s biggest memory of midwifery, so far, has been the day she delivered twins.
“I’ll never forget that day as long as I live,” she smiles. “The mother was fully dilated at 10cm when she came in, so it was panic stations, but we had everything set up and her first baby was born very soon; a lovely baby girl.
I delivered the little boy. The absolute delight in the room was infectious
“There were a couple of midwives and obstetricians in the room and the senior midwife then told the doctors to step back and let the midwife deliver the second baby, too.
“That was me and I delivered the little boy. The absolute delight in the room was infectious. You can’t describe the happiness and relief after the weeks of waiting for these babies. To leave the room that morning, seeing the mother smiling with her two babies in her arms was incredible. It’s making me a bit emotional just thinking about it!”
There is extra joy, too, for midwives and families, when safe deliveries are long-awaited.
“You get women who have had a couple of losses and this is their rainbow baby that comes into the world and everything is healthy and, well, that’s amazing to see, as well.”
Lows and highs
There are difficult days too, of course.
“With incredible highs of course there are lows,” she adds. “There can be pregnancy loss and late-term pregnancy loss, which unfortunately is part and parcel of life. Then, of course, you have other issues in all hospitals, like short staffing, and there are always emergencies and a little bit of panic at some point throughout the day.
The positives far outweigh the negatives
“But it all comes as part of working in a clinical setting. The team I work with in the Rotunda is amazing, though. That makes all the difference, so I’m very lucky.”
Darelle has no trouble summing up her attitude to her job: “The positives far outweigh the negatives. You come home after the busiest day but you know that somewhere you’ve made a difference to someone’s life.”
And yes, Darelle loves babies. “You wouldn’t do this job if you didn’t!” she says.
Irish Farmers Journal as a remedy
A colleague (who commuted from Cavan) would bring Darelle a copy of the Irish Farmers Journal during the lockdowns, which helped her cope with homesickness.
“She knew that it was hard to get the IFJ around Stoneybatter,” she says. “I really appreciated being able to sit of an evening, cup of tea in hand, reading it, feeling that bit of nostalgia and homeliness.”
Emily McAteer lives on a suckler farm near Nobber in Co Meath with her husband and parents and, at the time of this interview, it was a case of “the labour ward at work and the labour ward at home” as calving was still happening.
As with Darelle, growing up on a farm normalised birth for Emily, who is now a clinical midwife manager in Our Lady of Lourdes Hospital in Drogheda.

Emily McAteer is a midwife who lives on a suckler farm near Nobber, Co Meath.
“You’d be used to seeing cows calving and mares foaling, so birth was very familiar,” she says.
Emily went straight into midwifery training when she was 17 years old.
“I’m a direct-entry midwife and started my four-year course in midwifery in Dundalk IT,” she explains. “It’s a FETAC Level 8 degree. It’s an option that has been in existence for 10 years now, and mature students can apply, too. With this, you’re specialising straight away so it’s great if you’re sure that it’s what you want to do.”
Emily had a positive role model for midwifery in her family – her aunt had trained as a midwife in the UK. She also liked the insight into midwifery that the then-new TV series Call The Midwife provided, although she admits she may have had a slightly romanticised idea of the career.
I never thought of the complications that can arise – how unwell women can become at times
“At 17, you don’t have much life experience really,” she says. “Call The Midwife portrayed this kind of lovely normal and I only thought of normal birth, I suppose. I never thought of the complications that can arise – how unwell women can become at times.
“On-the-ward experience opened my eyes about how important our role is. Midwives are experts in normal pregnancy and labour, but you’re so important because you are the one that’s first detecting a deviation from that norm. You’re escalating it then and liaising with your multi-disciplinary team.
I just fell in love with midwifery
“That’s when your obstetric doctors come into play. I didn’t grasp all of that, initially, but getting a labour ward placement very quickly was a blessing. I felt like I got into the thick of it straight away. I just fell in love with midwifery then. It was an amazing experience and I think you know very quickly if it’s for you or not.”
Team effort
Emily qualified at the age of 21. “It is a lot of responsibility quite young,” she says, “but you have great support and, by that stage, you know what you’re about. It’s also very much a team effort here, with doctors and midwives working closely together. The autonomy you have is nice too.”
She also mentions the multicultural aspect of her job. “Ireland is such a diverse country now. We look after women from all over the world, so you learn about different cultures in relation to childbirth as you go.”
Emily believes that midwifery is a respected role and she is glad to see that men are now taking up midwifery as a career too.
“Midwife means ‘with woman’. You don’t have to be female to support a woman in childbirth. We need both sexes.”
Would do it all again
Emily has no doubt but that she would do it all again.
You just want to do your best
“The job is so rewarding. There are highs and lows like in any job but even on sad days you’re privileged to be in that room, supporting couples through. You are very much in the moment and you think, ‘If I was in this scenario how would I want to be treated?’
“That’s how I work,” she says. “You just want to do your best on the day for them. There are some very tough days, but women are amazing; so resilient and so strong. It’s a fantastic job.”
Pandemic challenge
The pandemic hasn’t been easy for midwives or new parents.
They both found the wearing of masks and PPE a huge challenge during the pandemic – for themselves and for new mothers.
“I suppose we’re all still a bit in shock about how it all occurred,” Emily says, “and it’s still ongoing but women and their families helped us so much by just being patient. It was so hard for new mammies and daddies with visitor restrictions as well but we look forward to it easing over time.”
Wednesday 5 May was the International Day of the Midwife.
For information about becoming a midwife click here.






SHARING OPTIONS